Implantation of the fertilized egg outside of the uterine cavity, usually in the Fallopian tube. Other locations (abdominal, ovarian, cervical) are less common. Predisposing factors are history of peritonitis or pelvic infection.
2.2.1 Diagnosis
Signs and symptoms
Symptoms common to tubal, abdominal or ovarian ectopic pregnancy:
- Recent history of intermittent abdominal pain, a few weeks of amenorrhea, which may be followed by vaginal bleeding or menstrual irregularity, nausea and vomiting, occasional dizziness or faintness.
- Examination: abdominal tenderness often unilateral; guarding, possible adnexal mass, cervical and posterior fornix tenderness.
In the event of tubal pregnancy:
- Blood may collect in the Fallopian tube (haematosalpinx). The symptoms above may then be more severe and prolonged, with a painful adnexal mass.
- Bleeding may gradually seep into the abdominal cavity over several days or weeks. The blood accumulates in the Pouch of Douglas and form a haematoma (haematocele). If a haematocele forms – especially if it is large – there may be other signs and symptoms:
- irritation of the bladder or rectum with urinary frequency, dysuria, rectal cramps and low grade fever;
- bulging and increased pain in the posterior fornix, with a pelvic mass with poorly defined borders and uneven consistency that pushes the uterus forward;
- anaemia.
In the event of sudden Fallopian tube rupture, the tube’s blood vessels are often damaged.
A haemoperitoneum (bloody effusion into the peritoneal cavity) develops quickly.
On examination:
- distended, tender abdomen, shifting dullness;
- exquisite pain in the Pouch of Douglas;
- scapular pain;
- hypovolaemic shock due to bleeding (rapid, weak or unmeasurable pulse, very low or unmeasurable blood pressure, tachypnoea, pallor, cold sensation, damp skin, agitation and anxiety).
In general, a cervical pregnancy (very rare) most closely resembles an incomplete abortion. It is often discovered due to massive bleeding during vacuum aspiration or curettage to evacuate the uterus.
Additional investigations
- Pregnancy test: usually positive; in case of haematocele, however, it may exceptionally be negative.
- Ultrasound: shows an empty uterus, and in some cases an adnexal mass (haematosalpinx or haematocele) or fluid/blood in the abdominal cavity (haemoperitoneum).
- If ultrasound is unavailable and there is still some doubt, culdocentesis (Pouch of Douglas puncture) may be useful to look for a haemoperitoneum. The procedure is pointless when laparotomy is clearly indicated.
- Culdocentesis:
- Perform general (ketamine) or local (1% lidocaine) anaesthesia.
- Swab the perineum, vagina and cervix with 10% povidone iodine.
- Push the posterior vaginal wall down using a speculum. Grasp the posterior lip of the cervix with Pozzi forceps and lift the cervix upward.
- Puncture the posterior fornix using a long, large-bore needle (e.g. spinal needle 20G) held as close to horizontal as possible, and aspirate with a 20-ml syringe.
- An aspirate containing non-clotting blood indicates haemoperitoneum.
Figure 2.1 - Puncture of the posterior fornix
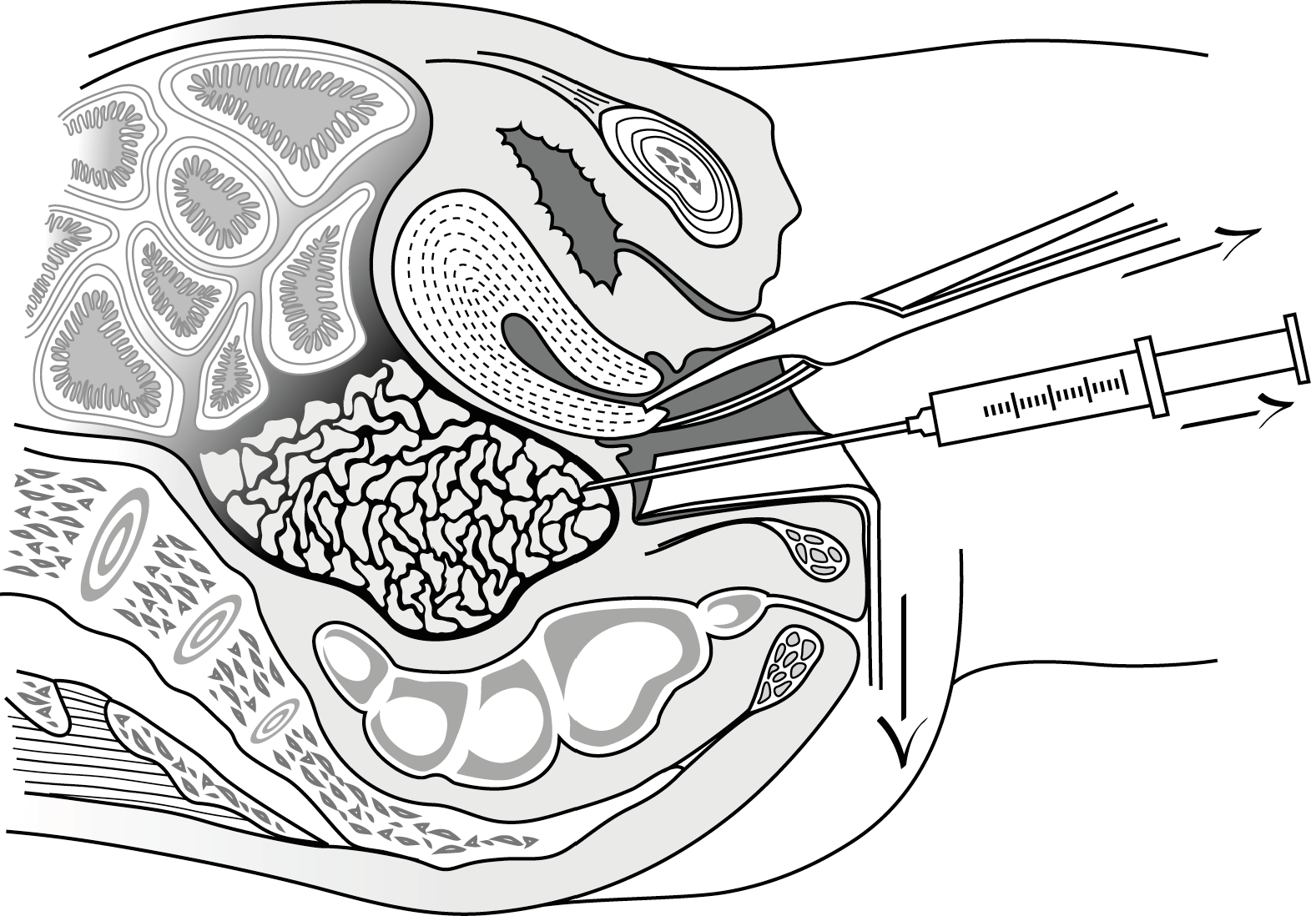
2.2.2 Differential diagnosis
The main differential diagnoses for ectopic pregnancies are abortion, salpingitis, ovarian abscess, appendicitis and diverticulitis.
When haematocele is suspected, also consider pyosalpinx, fibroma, or pelvic abscess from another cause.
When haemoperitoneum is suspected, also consider gastric or duodenal perforation or ovarian cyst rupture.
2.2.3 Management
When the diagnosis of ectopic pregnancy is highly likely:
- Prepare for laparotomy or refer urgently to a CEmONC facility.
- Insert an IV line (16-18G catheter) and administer Ringer lactate.
- Closely monitor: heart rate, blood pressure and bleeding.
- Prepare for a possible transfusion, determine the patient’s blood type, select potential donors or ensure that blood is available. If transfusion is necessary, only use blood that has been screened (HIV-1, HIV-2, hepatitis B, hepatitis C, syphilis, and malaria in endemic areas).
Special cases
- In case of cervical pregnancy, temporarily stop the bleeding, if possible, using intracervical Foley catheter compression or cerclage before considering total hysterectomy.
- Abdominal pregnancy is treated by laparotomy. Depending on its location, removing the placenta may be very difficult and cause severe bleeding; in that case, leave the placenta in place.