On this page
Rupture of the amniotic sac using an amnihook (or, if not available, the claw from half of a Kocher forceps).
5.3.1 Indications
- To speed up dilation if labour fails to progress.
- To speed up delivery once the cervix is fully dilated if labour fails to progress.
- As an adjunct to oxytocin for induction of labour (Chapter 7, Section 7.3.2).
- To try to stop the bleeding during labour in case of partial placenta praevia (be careful not to perforate the placenta).
5.3.2 Precautions
- Polyhydramnios (risk of cord prolapse): re-examine immediately after rupture to make sure that the cord did not end up below the presenting part.
- Use sterile technique (infection risk as a result of opening the amniotic cavity to pathogens).
5.3.3 Contra-indications
Absolute
- Complete placenta praevia
- Transverse lie
Relative
- Dilation less than 5 cm, irregular contractions (false labour, latent phase).
- Breech presentation prior to full dilation (keep the amniotic sac intact as long as possible).
- HIV or hepatitis B infection (or context of high-prevalence) prior to full dilation: keep the amniotic sac intact as long as possible to reduce the risk of mother-to-child transmission.
- Presenting part not engaged: risk of cord prolapse.
5.3.4 Technique
(Figure 5.10)
- Place the woman on her back with knees bent and thighs apart.
- Wear sterile gloves.
- Swab the perineum and the vagina with 10% povidone iodine.
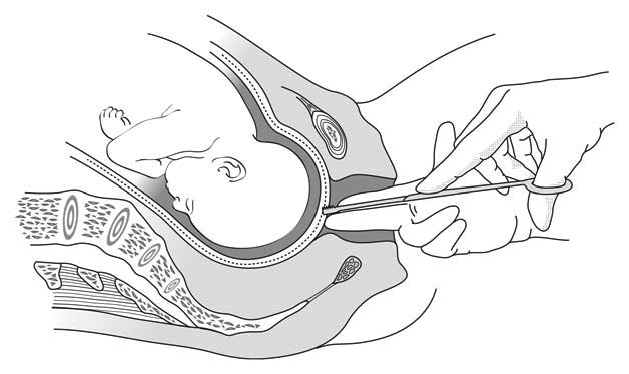
- With one hand, prepare access to the sac (hand well into the cervix). With the other hand, slide the amnihook between the fingers of the first hand—which spreads the vagina and the cervix and guides the tip—and make a small cut in the sac as it bulges during a contraction. Let the fluid drain slowly then, use a finger to enlarge the opening.
- Note the colour of the amniotic fluid (clear, greenish, or blood-stained). Isolated meconium staining, in the absence of an abnormal foetal heart rate, is not diagnostic of foetal distress, but requires closer monitoring.
- Make sure the cord has not prolapsed.
- Check the foetal heart rate before and after amniotomy.
Figure 5.10 - Artificial rupture of membranes